Just kidding, guys. I haven’t had a baby. And even if I had, I doubt I would have eaten the placenta. But I just couldn’t resist stealing the title of this NY Times blog post that happens to be the third result when I googled “placenta.”
Why was I googling “placenta”? Not for the pictures, that’s for sure!

Nick Baines ate his wife’s placenta… :\
I googled “placenta” to learn more about our gene-of-the-week: placenta-specific 1, or PLAC1.
While the topic of placentophagy is fascinating (IMO, humans stopped doing this for a reason, so why should we start now??1), it has nothing to do with PLAC1. At least not directly.
PLAC1 is an X-linked gene that is primarily expressed in cells derived from the trophoblast during embryonic development. PLAC1 is thought to be membrane-bound and seems to play an important role at the maternal-fetal interface. Plac1 knockout (KO, Xm-Xp- or Xm-Y) and heterozygous (Het, Xm-X) placentae with the Plac1-null allele inherited from the mother are about twice as large as wildtype (WT) placentae. The associated embryos are ~10% smaller, and the pups often do not survive beyond late gestation and weaning. Interestingly, Het placentae with the Plac1-null allele inherited from the father (XXp-) appear normal, due to paternal imprinting.2
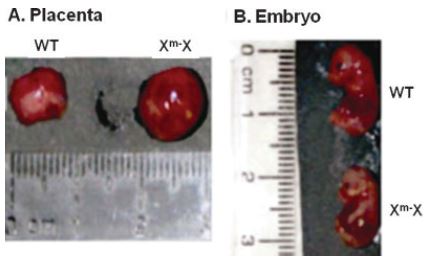
Gross appearance of a typical Het (Xm-X) placenta and embryo at E16.5. Plac1 ablation results in placentomegaly and intrauterine growth retardation (IUGR). (From Jackman et al., 2012.)
Recently, high levels of PLAC1 mRNA in maternal plasma were found to be a good potential marker for preeclampsia (which, spoiler alert, should mean something to Downton Abbey fans…).3 The authors hypothesize that the high levels of PLAC1 indicate abnormal interactions between trophoblast and uterine tissues, leading to placental insufficiency. (Seriously, reading this paper led me to rewatch a certain episode, and I totally cried! I cried because of this blog!)
Anyway, let’s talk about tumors. Developing embryos and tumors have a lot in common. In a recent study, Wang et al. reported that PLAC1 is expressed in a number of cancers.4 PLAC1 is localized on the surface of cancer cells and it may be a good “cancer/testis antigen,” which can be used for targeted immunotherapies. In both placental and tumor cells, PLAC1 may enhance survival by promoting growth factors, such as vascular endothelial growth factor (VEGF) and human chorionic gonadotrophin (hCG), and by suppressing immunological targeting by the mother’s or host’s immune system, but these are still only speculation.
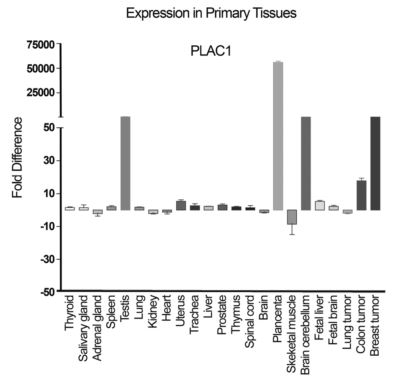
PLAC1 is highly expressed in placenta, as well as testis, the cerebellum, and several tumor cells. (From Wang et al., 2014)
Given the association of excess PLAC1 with bad things like preeclampsia and cancer, am I more worried about eating my placenta than I was before I started writing this post? Not necessarily (low levels of PLAC1 mRNA can also be scary5), but I’m with Nancy Redd… I’m not all that compelled to consume “an entity that had willingly left my body… once it comes out, maybe it should stay out.”
References
October is PLAC1 month. Last year, we learned that the absence of Plac1 in mice contributes to the development of hydrocephalus.6
- Young, S.M., Benyshek, D.C., and Lienard, P. (2012). The conspicuous absence of placenta consumption in human postpartum females: the fire hypothesis. Ecol. Food Nutr. 51, 198–217. [↩]
- Jackman, S.M., Kong, X., and Fant, M.E. (2012). Plac1 (placenta-specific 1) is essential for normal placental and embryonic development. Mol. Reprod. Dev. 79, 564–572. [↩]
- Zanello, M., Sekizawa, A., Purwosunu, Y., Curti, A., and Farina, A. (2014). Circulating mRNA for the PLAC1 Gene as a Second Trimester Marker (14-18 Weeks’ Gestation) in the Screening for Late Preeclampsia. Fetal Diagn. Ther. 36, 196–201. [↩]
- Wang, X., Baddoo, M.C., and Yin, Q. (2014). The placental specific gene, PLAC1, is induced by the Epstein-Barr virus and is expressed in human tumor cells. Virol. J. 11, 107. [↩]
- Farina, A., Rizzo, N., Concu, M., Banzola, I., Sekizawa, A., Grotti, S., and Carinci, P. (2005). Lower Maternal PLAC1 mRNA in Pregnancies Compli- cated with Vaginal Bleeding (Threatened Abortion <20 Weeks) and a Surviving Fetus. Clin. Chem. 51, 224–227. [↩]
- Kong, X., Jackman, S.M., and Fant, M.E. (2013). Plac1 (placenta-specific 1) is widely expressed during fetal development and is associated with a lethal form of hydrocephalus. Birth Defects Res. A. Clin. Mol. Teratol. 97, 571–577. [↩]

